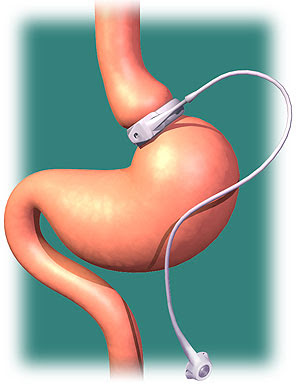
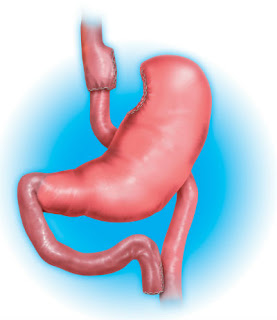
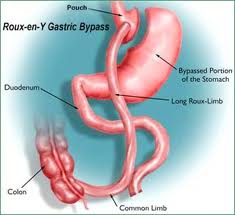
For an individual who is being considered for bariatric (weight loss) surgery for management of their obesity, it is becoming increasingly clear just how pivotal psychological issues are in the management before, during, and after the procedure. While there are many psychological benefits to bariatric surgery, there are also significant psychological risk that must be taken into careful consideration.
At the American Diabetes Association meeting in Orlando, FL, last week, I attended a lecture by Dr Lucy Faulkonbridge, Assistant Professor of Psychology at the University of Pennsylvania, who reviewed this topic for her audience.
There are many great things to be said about the psychological benefits of bariatric surgery. Bariatric surgery has been found to reduce depression and anxiety amongst individuals undergoing these procedures. The majority report improvement in body image, psychosocial functioning, and quality of life. Sexual function is also usually improved, as a consequence of many factors, including increased interest and improved mobility.
Having said the above, there are also potential negative consequences, some of which are absolutely devastating. While depression usually improves with weight loss, symptoms of depression can return, particularly in those who had significant depression prior to surgery. Importantly, while one study found that the risk of death was reduced by 40% at 7 years after gastric bypass surgery, they also found an increased risk of death from suicide and accidental deaths in this population.
Although bariatric surgery is typically very successful in achieving weight loss, the results can vary greatly from person to person. According to the landmark Swedish Obese Subjects’ Study , as many as 10% of gastric bypass and 25% of gastric banding patients are unable to maintain even a five percent weight reduction with surgery. (We do appreciate a 5% body weight reduction, as 5% weight loss in an obese individual decreases the risk of developing serious obesity-related complications such as heart disease, diabetes, and cancer.) Interestingly, the success of weight loss surgery seems to depend in part on psychological issues. While a background of psychological issues in a general sense is not predictive of degree of weight loss, active symptoms of depression or a tendency towards binge eating prior to surgery tends to result in smaller weight losses after surgery.
Although the literature in this area is somewhat conflicting, Dr Faulkonbridge postulated that while distress related to psychological illness may be an impediment to the success of bariatric surgery, distress related to extreme obesity may be a predictor of greater success, as this distress should improve with weight loss. The key is to determine what the source (or sources) of distress is/are prior to surgery, such that these issues can be addressed and dealt with prior to surgery, in order to optimize the medical and psychological outcomes of the procedure.
The psychology behind post operative exercise routines may play a part, too. In patients who have had gastric banding, those who did not increase their activity level after surgery are much more likely to have weight regain than those who do become more active post operatively. There is also some data to suggest that some patients may actually engage in less physical activity after the surgery, despite having shed pounds and most often enjoying increased mobility. Having an exercise program established prior to surgery is an important component to maintaining long term success with these permanent lifestyle changes as well.
Follow up patterns with the surgeon was also identified as being associated with weight loss success. While only 40% of patients return for their annual visits with their surgeon after their operation, it is these patients who seem to have the best weight loss success. The relationship between weight loss success and compliance with follow up is likely multifactorial.
It is clear that psychological issues must be taken into very serious consideration prior to, during, and after bariatric surgery. Key points to highlight include:
1. Thorough psychological evaluation and counseling before bariatric surgery is paramount. This should ideally take place in the form of screening questionnaires, as well as counseling and support from mental health care professionals. It is important that active mental health issues are dealt with as well as possible prior to surgery, to provide the greatest chance of success. It is noted that some people may not be appropriate candidates for bariatric surgery if their psychological issues are not stable or well managed.
Ideally, this process should take place as part of a team approach to preparation for bariatric surgery, including help from dieticians, nurses, physicians, and occupational therapists. Psychological support is also crucially important towards preparation for the permanent lifestyle change that defines bariatric surgery (very small portion sizes, alteration in food preferences, and a permanent change in one’s relationship with food).
2. Psychological support and access to mental health professionals through and following the bariatric procedure, both short term and long term. The needs of the individual patient will vary greatly – it is the availability, and experience of health care professionals in dealing with the issues that may arise, which are key.
3. Support from friends and family throughout the process. A solid support network provides outlets to deal with emotional issues that may arise. It is important that a patient’s loved ones are accepting and understanding of the motivations behind bariatric surgery, and are equally prepared to both endure the trials, and celebrate the tribulations, that may lay along the path towards successful weight loss.
Dr. Sue © 2010 www.drsue.ca drsuetalks@gmail.com