One of the main reasons why long term blood sugar control is so important in diabetes is the prevention of diabetes complications. Diabetic neuropathy, which is damage to nerves caused by chronic elevation in blood sugars, is one of the complications we are trying to prevent. Diabetic neuropathy affects a lot of people (you may be surprised by just how many – read on!), can be present in people who don’t even have diabetes yet, can take many different forms, and can have a profound impact on the quality of life of people living with diabetes.
The American Diabetes Association has recently released a Position Statement (download is free) to help guide clinicians in understanding, diagnosing, preventing, and managing this complication of diabetes.
Some key points from this article:
1. Diabetic neuropathy (DN) is a diagnosis of exclusion. In other words, just because a patient with diabetes has findings of neuropathy, doesn’t mean that the diabetes is necessarily the cause. Other causes of neuropathy (discussed in the article) need to be ruled out before the nerve problem is attributed to diabetes as the cause.
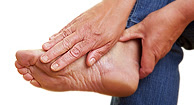
2. There are many types of diabetic neuropathy. Distal symmetric polyneuropathy usually starts with symptoms in the feet, including numbness, tingling, pain, and burning, especially at night. Autonomic neuropathies can affect/include the heart, ability to maintain blood pressure when standing up (orthostatic hypotension), the gastrointestinal tract, urinary tract, sexual dysfunction, or dysfunction in sweating. There are also forms of diabetic neuropathy that can affect specific nerves (cranial or peripheral), or bundles of nerves as they exit the spinal column.
3. Diabetic neuropathy is common. Distal symmetric polyneuropathy affects 50% of people with type 2 diabetes after 10 years, and 20% of people with type 1 diabetes after 20 years. Autonomic neuropathy involving the heart may affect up to 60% of people with type 2 diabetes after 15 years, and up to 30% of people with type 1 diabetes after 20 years.
4. Diabetic neuropathy can be present in people with prediabetes. Distal symmetric polyneuropathy may be present in 10-30% of people with impaired glucose tolerance, and autonomic neuropathy affecting the heart has been found in people with impaired glucose tolerance as well.
5. Prevention of diabetic neuropathy is key, as there is no effective treatment available for established nerve damage. Prevention is achieved primarily through optimizing blood sugar control. Lifestyle interventions are recommended for prevention in people with prediabetes or type 2 diabetes, and a multifaceted approach including targeting of cardiovascular risk factors is recommended for prevention of cardiac autonomic neuropathy in people with type 2 diabetes.
6. Management of established diabetic neuropathy is directed towards the particular type of neuropathy each patient has. This can include pain control medication, fall prevention, and specific treatments to manage symptoms of the autonomic neuropathies.