(my less-than-happy emoji face)
Prefer to listen? Check out my podcast here!
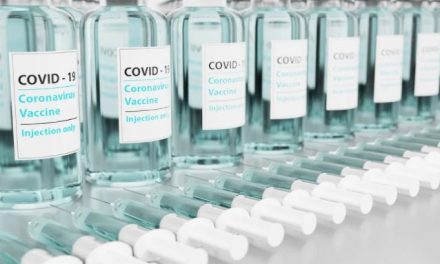
As the word about the efficacy of new and emerging obesity/diabetes medications continues to spread, the global shortages of these medications continues. The medications we are talking about here are the GLP1 receptor agonist semaglutide (Wegovy for weight management, Ozempic for diabetes) and the dual GIP/GLP1 receptor agonist tirzepatide (Zepbound for obesity, Mounjaro for diabetes).
In many countries, Ozempic and Mounjaro (diabetes brands) have been available but Wegovy and Zepbound (weight management brands) have not, so doctors have been prescribing Ozempic and/or Mounjaro for weight management. As blogged previously, some countries have responded by allowing access only to people with type 2 diabetes, and denying access to people with obesity who don’t have diabetes.
A Perspsective article in The New England Journal of Medicine suggests a different approach. Authors propose a ‘fair-allocation’ framework as to who should be prescribed these medications first, during times of shortage. They suggest four tiers of priority for who should get medication:
Tier 1. Objective: Minimize potential years of life lost by preventing excess and premature death.
- people with body mass index (BMI) ≥40 kg/m2
- people with ‘severe’ type 2 diabetes (A1C >8%), whose disease hasn’t responded to alternative treatment
Tier 2. Objective: Prevent imminent medical complications such as cardiovascular events.
- people with BMI 35-39.9 kg/m2
- followed by people with ‘severe’ type 2 diabetes (A1C >8%)
Tier 3: Objective: Prevent future medical complications, such as cardiovascular events.
- people with BMI 30-34.9 kg/m2
- followed by people wtih type 2 diabetes (A1C >7%), whose disease hasn’t responded to alternative treatment
Tier 4. Objective: Improve quality of life and social and emotional health.
- people with BMI 25-29.9 kg/m2
- or people with type 2 diabetes and A1C >7%, who aren’t eligible under another tier
All four tiers are further broken down into two phases, to prioritize younger patients first:
- phase 1: younger patients (eg <50 years)
- phase 2: older patients
In Tiers 2-4 , they suggest putting priority on obesity before diabetes, as treating obesity offers the opportunity to prevent or delay diabetes, and because many other treatments for diabetes exist, whereas the choices for obesity medication are few. The authors are also in favor of exempting existing users who are taking these medications for health benefits from this tiered system – ie , not taking away treatment for those already on treatment (which is great).
While I am glad that authors are suggesting a paradigm that embraces obesity as a chronic disease that should not be put in second place behind diabetes for need of treatment, I have concerns about the tiers suggested.
First, BMI is not a marker of the severity of the disease of obesity. BMI is simply a calculation based on weight and height. One person with a BMI of 42 may be quite healthy overall, while another person with a BMI of 32 may be struggling with sleep apnea, fatty liver disease with scarring (fibrosis), and hypertension (as examples). Severity of obesity is defined by the health complications associated with elevated weight and how elevated weight is impacting that person’s quality of life. In our Canadian Obesity Clinical Practice Guidelines, the Edmonton Obesity Staging System (EOSS) is suggested to determine the severity of obesity and guide clinical decision making. The EOSS is a measure of the mental, metabolic, and physical impact that obesity has on the person’s health, and uses these factors to determine their stage of obesity, from stage 0 to stage 4 (see table 3, page 6 from our Guidelines here).
As regards the A1c (diabetes control) criteria, it is true that a higher A1c is associated with a higher risk of complications over time. However, the ‘severity’ of diabetes is not determined by A1c, but rather, by the burden of health complications related to diabetes. Further, the multiple health benefits of the GLP1 receptor agonists beyond diabetes control are in part independent of glucose control (eg reduction in heart attack/stroke risk – more on this below).
Third, both the BMI and A1c criteria could be perceived as effectively ‘punishing’ those who are having some success to control weight or A1c by way of their dedication and hard work on their health, because their BMI or A1c aren’t ‘high enough’ to get into a higher tier. The thinking of a patient could follow: ‘Well, does that mean if I gain 15lbs more, or stop my insulin to get my A1c higher, then maybe I can get access to the GLP1 medication?’
I am also concerned about the objectives of each tier. These objectives assume that a higher BMI is the obesity metric that should be used to define how sick, or how high a health risk, that person has. Again I come back to how heterogeneous the disease of obesity is. Some people with a BMI of (for example) 29 or 31 present with obesity-related health issues that are much more advanced, and would put them squarely within the Tier 1 objective, than other people who have a BMI of 40 or higher but don’t yet have much obesity related disease.
These criteria also don’t take into account whether a person already has cardiovascular (CV) disease. Several GLP1 based medications have shown the capacity to reduce CV events in people with type 2 diabetes [including semaglutide (Ozempic), liraglutide (Victoza), and dulaglutide (Trulicity)], and Wegovy has shown the capacity to reduce CV event risk by 20% in people with cardiovascular disease and obesity without diabetes. People with existing cardiovascular disease are at highest risk of having a heart attack or stroke, yet there is no priority set for these people to have higher priority of access to medication.
Access being granted to younger people before older people is a strategy that authors suggest, with the thinking that intervening in a younger person’s life will improve their health starting earlier, giving them a longer number of healthier years. I can appreciate the logic here, but at the same time, I do not want to deprive my 50+ patients from access due to yet another numerical stratification. This is where I throw my hands up in frustration, because the unfortunate reality is that there is no perfect way to fairly allocate this restricted resource. Argh.
BOTTOM LINE: The global shortage of GLP1 based medications presents major challenges for people (and their health care providers) who need or already depend on these medications to improve, manage, and/or maintain health. It is very difficult to figure out who should get priority for new prescriptions when demand drastically oustrips the supply. I (and authors of this article) sit strongly in the camp that obesity and diabetes are both chronic diseases that need treatment. If priorities must be set for who gets higher priority for a new start, in my opinion, stratification should be geared more towards people who have a greater burden of health issues related to weight or diabetes that could benefit, and not by a set of numbers. As supply catches up with demand, and as other new highly effective medications hopefully enter the market soon, I look very forward to the supply issue being put firmly in the past.
Disclaimer: I receive honoraria as a continuing medical education speaker and consultant from the maker of semaglutide and liraglutide (Novo Nordisk), and tirzepatide and dulagutide (Eli Lilly). I am/have been an investigator in clinical trials of semaglutide, tirzepatide, and liraglutide.
Check me out on X/twitter! @drsuepedersen
Share this blog post using your favorite social media link below!
www.drsue.ca © 2024