Weight loss surgery, or bariatric surgery as it’s called, is one hot topic in the obesity world. And I have lots to say about it, as it is the main focus of my research during my year-long sabbatical here at the University of Copenhagen. Here’s a little introduction….
Desperate times call for desperate measures. We exist in a global society that has seen an explosion of obesity in the last few decades. The majority of Canadian adults are overweight at a staggering 59%, with one in four being clinically obese.
The treatment of overweight and obesity must be approached on an individual basis. For most people, obesity has its roots in lifestyle problems, and as such, adopting a new paradigm of lifestyle is the best solution. However, for some people, this seems to be beyond reach. For some people, medications for treating obesity can result in successful weight loss, though they may not be effective for long term weight loss, particularly if not accompanied by lifestyle alterations. For those individuals who are severely overweight, and have not been successful with intensive attempts at lifestyle alteration and/or medical therapy, surgery may be the most appropriate option.
At present, bariatric sugery is a treatment that is reserved for people with very severe, or very complicated obesity.
Commonly accepted criteria for qualifications for surgery include:
-
- A BMI (body mass index) of 40 or more; or
- a BMI of 35 or more, PLUS either type 2 diabetes, high blood pressure, or obstructive sleep apnea (as complications of obesity)
(You can calculate your BMI using the BMI calculator on my website, in the right hand column https://www.drsue.ca/)
- LAGB involves putting an inflatable ring around the stomach near the top of the stomach, such that it restricts the size of the stomach.
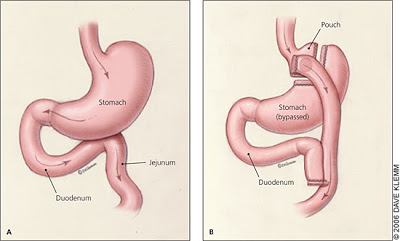
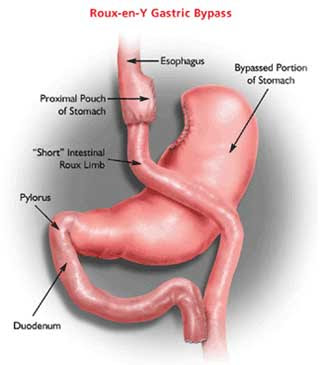
- RYGB is more complex surgery in which the stomach is made smaller, and part of the small intestine is also bypassed, thereby reducing both the amount of food a person can intake, as well as the capacity to absorb that food (diagram displayed above).
Is this topic of interest to you? Email drsuetalks@gmail.com if you’d like to hear more.