Canada, like the rest of the world, is caught in a diabetes epidemic. Over 2 million Canadians are diagnosed with the disease, and by the year 2020, those numbers are expected to rise to 3.7 million. This epidemic is paralleled by the high prevalence of obesity, which currently affects 25% of Canadian adults and 10% of Canadian children. One of the treatment options that is being increasingly considered to treat type 2 diabetes in the setting of severe obesity is weight loss surgery.
I attended the First Canadian Diabetes Surgery Summit in Montreal this week, hosted by McGill University, to discuss this very issue. Over two very intense and productive days, a collection of international leaders in the area presented their research and clinical experience to a diverse group including Canadian surgeons, family physicians, endocrinologists, health care professionals, and policy makers. A wealth of learning, sharing, and ideas were generated from this summit, of which I am going to discuss over the course of several articles in the coming weeks. Here are the highlights.
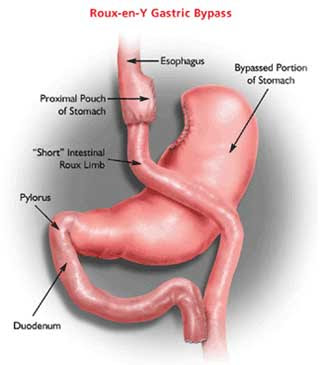
In short, bariatric surgery is a very effective treatment for type 2 diabetes. The results depend on the type of surgery done, but remission rates of diabetes of over 80% have been documented, and sustained for at least 2 years. Much of this success is related to the impressive weight loss that is seen with bariatric surgery, but gut hormone changes with certain types of surgery (such as gastric bypass surgery) play an important role as well.
It must be emphasized that bariatric surgery is only appropriate for a very select group of people. The current guidelines recommend bariatric surgery as a potential option for patients with a BMI >40, or a BMI >35 with at least one serious medical complication (such as diabetes), who have failed intensive attempts at weight loss with conventional treatments (lifestyle alteration, medications, etc). Bariatric surgery has a long list of potential side effects and complications that must be seriously considered, and which vary depending on the type of surgery performed. On balance, however, bariatric surgery has been shown to decrease mortality by 28-40% in this population, and as such, may be the most appropriate option for some people.
In Canada, we struggle with very limited accessibility to bariatric surgery. As Dr. Nicolas Christou, one of Canada’s leaders in bariatric surgery, pointed out:
- Based on very conservative estimates that 5% of the 1 million Canadians who fit criteria for bariatric surgery would actually be appropriate candidates for surgery, 50,000 Canadians would currently be candidates for the procedure.
- Approximately 3,000 bariatric procedures will be done in Canada this year.
- According to these numbers, then, Canada currently has in excess of a 15 year back log of patients who could benefit from these procedures.
What can we do about this? The problem of course, is funding. Funding for bariatric surgery is extremely limited in Canada, though accessibility does vary greatly by province. Cost analyses suggest that for patients with diabetes, the costs of bariatric surgery to the government are recouped by 26-30 months post operatively, and after that, there are only savings to be had by the health care system due to the decreased rate of diabetes related complications, hospitalizations, and medication requirements of these patients.
On balance, increased accessibility to bariatric surgery in Canada, provided in the appropriate clinical setting by a multidisciplinary, experienced health care team, should be discussed amongst Canadian health care professionals, patients, and the general public.
Dr. Sue © 2010 www.drsue.ca drsuetalks@gmail.com