Our knowledge and understanding about the role of gut hormones in type 2 diabetes continues to grow, as we get a better understanding of the mechanisms involved in the often dramatic improvement in diabetes that is seen after bariatric surgery. In gastric bypass surgery, we know that at least one of the mechanisms involved is food literally bypassing the first segment of the small intestine, called the duodenum. This effect may be seen because food is more rapidly delivered to the intestine further down, causing a more powerful release of hormones from the more distal intestine (called the hindgut hypothesis). However, there may also be an as yet unidentified hormone (or hormones) secreted by the first part of the gut that have an antidiabetic effect, and by having food skip over this part of the gut, this mystery antidiabetic hormone is not released, thereby improving blood sugar control (called the foregut hypothesis). We do know that the surface of the duodenum in a person with diabetes is altered, with a sort of overgrowth of cells in the duodenal mucosal (called hypertrophy and hyperplasia).
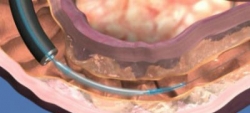
For believers of the foregut hypothesis, a novel approach called Duodenal Mucosal Resurfacing (DMR) is now being studied to see if diabetes control can be improved by doing a sort of ‘thinning out’ of the lining of the upper part of the intestine.
The first human study of DMR, recently published in the journal Diabetes Care, performed the DMR procedure in 39 patients with type 2 diabetes. They found an improvement in diabetes control at 6 months post procedure, with greater improvement in those who had a longer segment of the duodenum ablated than those that had a shorter segment treated. Improvement in blood sugars was seen as soon as 1-2 weeks after the procedure, despite no restrictions in diet or calorie intake being recommended. The improvement in diabetes control was not as powerful as what is seen with gastric bypass surgery, suggesting that there are many additional elements at work in gastric bypass surgery. The authors also noted that there was some erosion of the improvement in diabetes control at 6 months, so certainly larger and longer studies need to be done to understand what the effect of this procedure is over the long term. There was little weight loss in this study (only a few kg), so the DMR does not hold promise as a weight management strategy. The procedure was well tolerated overall, though there were three cases of duodenal stenosis that were treated with balloon dilatation. The authors noted no signals for malabsorption (eg no calcium abnormalities or iron deficiency anemia), but this would need to be evaluated carefully in long term studies as well.
It will be interesting to see further study of the DMR procedure.