In the outdated and incorrect view that people who struggle with weight can simply lose weight by ‘eating less and moving more’, one of the the most important and overlooked contributors to weight struggles is mental health issues.
The relationship between obesity and mental health is complex and goes both ways: not only can mental health issues contribute to weight gain, but weight gain can exacerbate or even bring on mental health concerns. People with mental health issues and obesity are often subject to compounded bias and stigmatization against both medical conditions, which can have a profound negative impact on the care they receive. If mental health issues related to weight are not addressed, they can be a barrier to effective weight management.
Here are some of the highlights from the Mental Health Chapter in the 2020 Canadian Adult Obesity Guidelines:
For any person seeking treatment for obesity, it is important to consider whether any mental health issues may be coexisting (cause or effect), with a focus on looking for possible depression, binge eating disorder, and/or ADHD.
All too often, medications for mental health issues are started without regard for their effect on a person’s weight. Amongst antidepressant, antipsychotic, and antiseizure medications, there are some that cause substantial weight gain, some that are weight neutral, and some that can even help with weight loss. Thus, effect on weight should be considered when these medications are being prescribed. If a medication that causes weight gain is being used, it is important to monitor weight, blood sugars, cholesterol, and other metabolic/cardiovascular health parameters. (note: check out the awesome Table that lists medications that cause weight gain, and alternatives that don’t, in the Assessment chapter of the Guidelines – Table 8, page 14)
Psychological intervention, one of the Three Pillars Of Obesity Management, can be effective in managing weight in people who also have mental illness. The intensity of the behavioural intervention will need to increase for people with more severe mental illness. (note: psychological and behavioral interventions are covered in their own chapter, which I will review separately in an upcoming blog post)
Metformin is recommended for prevention of weight gain in people with severe mental illness being treated with antipsychotic agents that are associated with weight gain. (grade A, level 1 recommendation) (note: this strategy is particularly effective if metformin is started at the same time, or soon after, the antipsychotic medication is started)
Of weight management medications available in Canada, the GLP1 receptor agonist liraglutide has the most safety and efficacy evidence in people with obesity on antipsychotic medication. (note: medications for treatment of obesity are covered in their own chapter, which I will review separately in an upcoming blog post)
For people with overweight or obesity and binge eating disorder, lisdexamfetamine (Vyvanse) and topiramate (Topamax) should be considered as part of the treatment strategy.
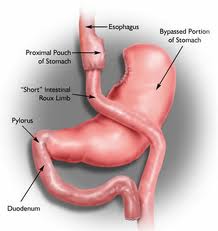
Before bariatric surgery, it is important to assess for any mental health issues. The presence of an active psychiatric disorder does not mean that bariatric surgery shouldn’t be done, but warrants further assessment of potential impact on long-term weight loss.
After bariatric surgery, ongoing psychological assessment and support is important. It is important to monitor for any substance use changes (eg alcohol), as there is an increased risk of substance abuse after bariatric surgery. It is also important to monitor for any self harm risk, as increases in suicide and self harm have been reported after bariatric surgery.
NOTE: This blog is not intended to be a full synopsis of the chapter. There is a wealth of information in this chapter that is beyond the scope of one blog post. I encourage everyone to read the recommendations and key messages in full, and to dig in to the entire chapter!
Stay tuned for much more on the Obesity Guidelines in coming weeks!
Share this blog post using your favorite social media link below!
Follow me on twitter! @drsuepedersen
www.drsue.ca © 2020