As blogged previously, bariatric (weight loss) surgery is a treatment options for people with severe obesity that has proven to be resistant to treatment with more traditional and conservative measures. The treatment does not end with the surgery itself, however – the story is far more complex than that.
As beautifully summarized in the Patient Guide to Endocrine and Nutritional Management after Bariatric Surgery in the Journal of Clinical Endocrinology and Metabolism (a free download!), there are several aspects which require close attention and follow up in order to minimize the chance of weight regain after surgery, to minimize the risk of developing a complication of bariatric surgery, and to ensure that complications of obesity are well managed postoperatively.
To decrease the chance of weight regain after surgery, a lot of the preventive work actually has to happen before the surgery is even done. It must be recognized, as with any ‘diet’, that the lifestyle change being made has to be a permanent one. This is not about eating smaller portions or altering food choices for a short period of time – this is forever. It is also absolutely critical that the relationship with food is thoroughly explored and managed well before the surgery takes place. There are many contributing factors to overeating, many of them emotional: eating in sadness, in joy, to comfort, to alleviate stress, even to service a true addiction to food. People who have not had help in dealing with these aspects of their weight struggles, or who have not worked through these issues prior to surgery, are not appropriate candidates for bariatric surgery, as they stand a high risk of weight regain postoperatively if those habits and coping mechanisms are not managed beforehand.
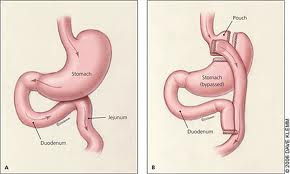
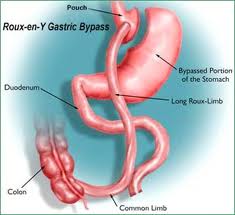
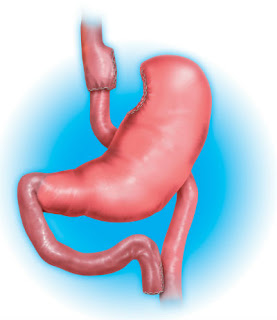
The risk of nutritional deficiencies is very real after bariatric surgery, particularly after gastric bypass surgery (pictured above), which involves a re-routing of the small intestine such that about 1.5 meters of small intestine is no longer exposed to food and the enzymes required to digest it. Patients who undergo gastric bypass surgery are at risk of life threatening complications if they do not adhere to their supplement regimen, which for most patients includes a specific multivitamin, calcium, vitamin B12, vitamin D, and often iron. An individual who is committed to having gastric bypass surgery must be equally committed to taking supplementation for the rest of their lives. Protein malnutrition is a potentially severe complication of any type of bariatric surgery due to decreased intake; it is essential to follow the protein consumption recommendations provided by the bariatric program’s dietician (usually at least 90 grams of protein intake per day).
Because bariatric surgery often has a profound beneficial impact on several obesity-related complications such as diabetes, high blood pressure, obstructive sleep apnea, cholesterol, and osteoarthritis (to name a few), it is important to have physicians involved both pre- and post-operatively who can help to manage changes in medications and treatment approach that are often necessary.
While bariatric surgery is a very appropriate treatment option for some people, it must always be remembered that bariatric surgery is not a quick fix or a cure; it is the exchange of one set of medical issues for another (though usually in a positive direction), and it is most certainly a permanent lifestyle alteration.
Dr Sue Pedersen www.drsue.ca © 2010 drsuetalks@gmail.com
Follow me on Twitter for daily tips! @drsuepedersen